 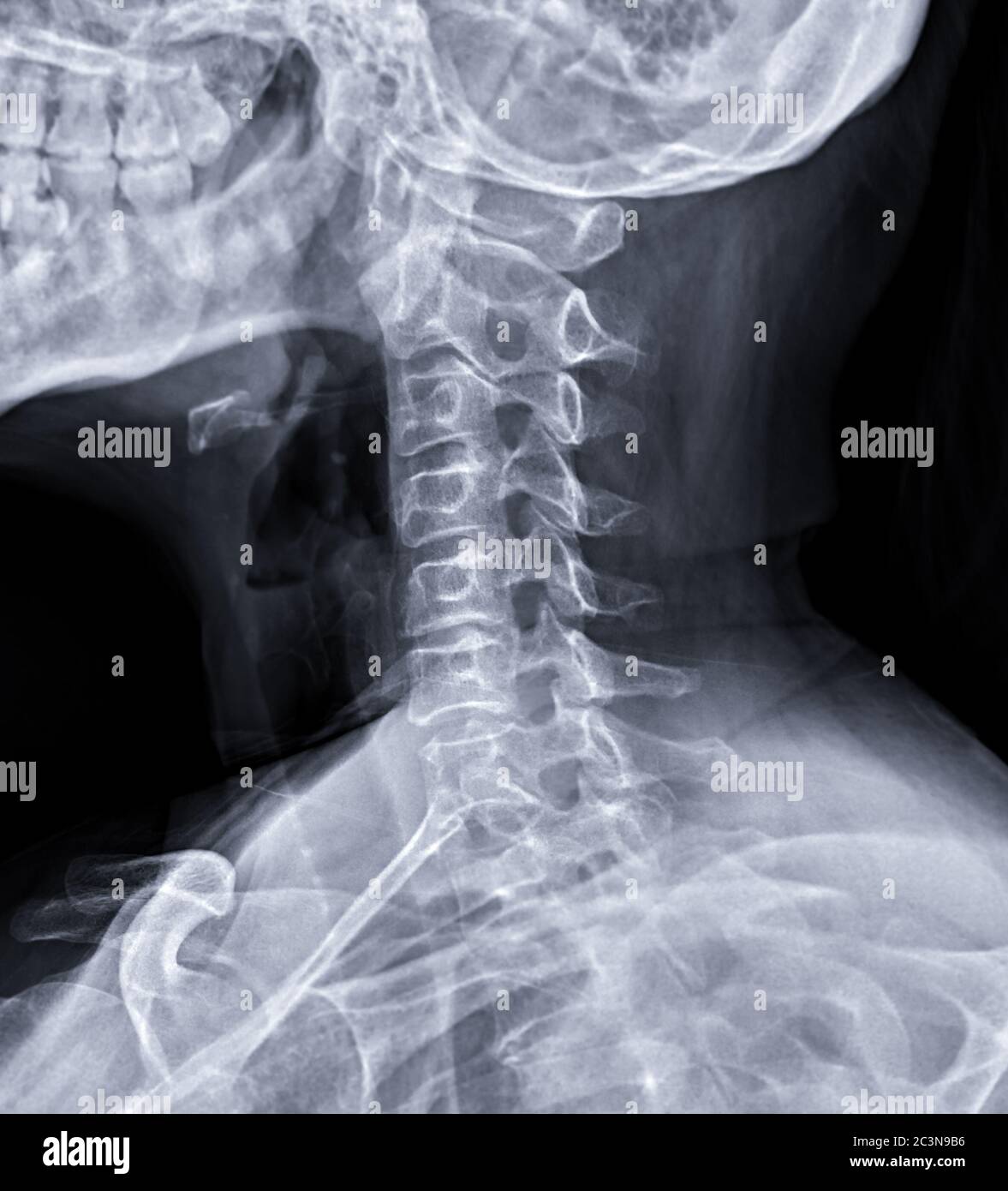 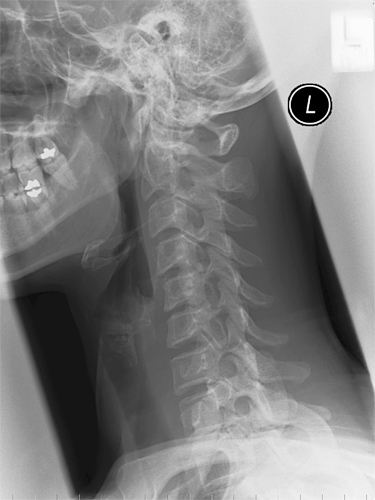
This permitted coronal and sagittal reconstructions of the entire length of the cervical spine in addition to the standard axial images. Computed tomography (CT) was first introduced in the 1970s but did not prove adequate for the evaluation of the acutely injured spine until the early 2000s with the introduction and perfection of multidetector CT (MDCT), with rapid exposures coupled with the development of immediate and readily accomplished multiplanar image reconstructions. Though traditional and long the mainstay of cervical spine evaluation, radiographs of the cervical spine now have a limited role in the initial assessment of cervical spine trauma. Teardrop fractures at anterior margins of vertebral bodiesĬlosely evaluate prevertebral soft tissues for swelling. Spondylosis and degenerative changes in elderlyĬheck for evidence of hyperextension injury. Obtain an MRI for those with neurologic signs and symptoms.Ĭheck width of spinal canal for spinal stenosis. Where to look when you see nothing at all Two- or three-level fractures encountered in 20% of spinal fracturesĬT entire T and L spine after identifying fracture of C-spineįind a compression fracture: look for associated posterior element injury.įind a vertebral body injury: look for bony compromise of spinal canal.įind a facet malalignment on one side: look for contralateral facet malalignment/fracture. Where else to look when you see something obviousįind an injury at one level: closely evaluate the entire cervical spine above and below.įractures of C1 and C2 often associated with fractures of the lower cervical spine (C4-C7) Subtle fractures on radiography – need CT Relatively more involve lower cervical spine, C4-C7 Spinal cord injury without radiographic abnormality (SCIWORA)Īt and beyond 14 years of age injuries similar to those of adults Rare – apophyseal separations of synchondrosis between dens and body of C2 Relatively more involve upper cervical spine Often with either subtle or even without overt radiographic abnormality (SCIWORA)įracture of inferior or superior anterior margins of vertebral bodyįracture of osteophyte at superior or inferior anterior margin of vertebral bodyįractures in DISH (diffuse idiopathic skeletal hyperostosis)Ĭommon sites of injury in children and adolescentsĬervical spine injury ( CSI) rare in children under 8 years of age Spinal cord injury in presence of significant degenerative arthritis and disc disease 
Intervertebral disc, joint capsules, and interspinous ligamentĪnterior and posterior longitudinal ligamentsįacets – unilateral or bilateral – rotation, shearing injuries Vertical sagittal split of vertebral body Jefferson fracture – fractures of ring anterior and posteriorĬ2 pars interarticularis fractures – hangman’s fractureĬompression, distraction, and translation/rotation injuries (SLIC) Using the standardised technique to obtain oblique radiographs of the equine cervical vertebrae may provide additional diagnostic information about the APJ.Axial, sagittal, and coronal noncontrast images in bone algorithmĮxtending through at least the level of T1Īxial and sagittal images in soft tissue algorithmĬraniocervical junction (Skull base – C2) The description of the normal radiographic anatomy of the cervical APJ of the caudal neck region in horses provides a valuable reference for the interpretation of cervical radiographs. Obtaining oblique radiographs within the specified range of angles resulted in a consistent radiographic image of the APJ in the caudal cervical region in the live individual. 
The optimal range of angles for obtaining oblique radiographs was 50-55 degrees for C4-5, 45-55 degrees for C5-6 and 45-5 degrees for C6-7. The radiopaque markers facilitated identification of the APJ by clearly outlining the margins of the cranial and caudal articular processes on lateral and oblique radiographs. Lateral and oblique radiographs of the caudal neck were obtained in 6 live horses under standing sedation to assess the feasibility of the technique. A novel cineradiographic technique was employed to determine the optimal oblique projection to permit both left and right APJ to be assessed on the same radiograph. Radiopaque markers were used to highlight the contours of the APJ on both lateral and oblique radiographs. To determine the optimal technique for obtaining oblique radiographs of the APJ of the caudal cervical vertebrae (C4-5, C5-6 and C6-7) and to provide a detailed description of their normal radiographic appearance, on both lateral and oblique radiographic projections. Plain radiography is the standard imaging technique for investigation of diseases associated with the articular process joints (APJ) of the caudal neck however, the radiographic anatomy of these structures on both lateral and oblique radiographic projections has not previously been described in detail. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
